How cystic fibrosis (CF) affects the lungs
The lungs contain a network of tubes that divide into smaller and smaller tubes as you go deeper inside them. These tubes are called airways. The airways are covered with fine hair-like projections called cilia, which constantly sway back and forth to sweep thin, watery mucus up and out of the airways.1
Airways of a person without CF
In normal lungs, thin and watery mucus traps dirt and germs that might cause an infection. The cilia sweep the mucus out of the lungs and up towards your windpipe, where it is coughed up. This results in the germs being expelled (removed from the body).1
For cilia to be able to sweep mucus out of the lungs, the inside of the airways needs to be moist. This allows the cilia to move back and forth freely.2


Airways of a person with CF
In people with CF, the number and/or function of cystic fibrosis transmembrane conductance regulator (CFTR) proteins is reduced. These proteins help to make sure we have the correct balance of salt and water in our organs. When this balance isn’t right, thick and sticky mucus may be produced. This makes it difficult for the cilia to move freely and sweep mucus from the lungs.2,3


If cilia can’t move freely, mucus and germs can build up, leading to the symptoms of CF, which include:
- Wheezing3
- Shortness of breath3
- A persistent cough that produces thick phlegm (sputum)3
- Lung infections including pneumonia and bronchitis3
- Bronchiectasis (damage to the airways that causes them to become wider, making it harder to move air in and out as you breathe, and harder to clear mucus)4
The build-up of mucus and germs can lead to pulmonary exacerbations. Pulmonary exacerbations are times when symptoms get worse – this may mean that for a period of time the lungs aren’t working as well as they usually do.4 During a pulmonary exacerbation, people may cough more, produce more mucus, notice a change in the colour of their mucus, lose their appetite and experience weight loss.5 In some cases, people suffering from a pulmonary exacerbations might need treatment with antibiotics and may need to stay in hospital for a few days.4
The CFTR protein, which is faulty in people with CF, is found on the surface of cells in many organs and tissues throughout the body. This means that people with CF can experience a wide range of symptoms. These symptoms, how severe they are and which organs in your body are most affected can vary a lot between people with CF.4 This variation is the result of each person’s individual type of defect (mutation) within their CFTR gene (their genotype) and their surroundings.6
How CF affects the digestive system
The role of the digestive system

The process of digestion involves breaking down the food you eat to absorb the nutrients it contains. This process begins in your mouth and continues as the food passes down into your stomach and small intestine, where the pancreas helps digest the food further so your body can use the nutrients in it. Finally, the unusable bits of the food you ate reach the large intestine and rectum, where they move out of your body.7
In CF, sticky mucus in the pancreas interferes with the proper digestion of your food and causes blockages in the intestines. 7
The pancreas
The pancreas plays an important role in breaking down and absorbing nutrients and one of its main jobs is to make enzymes. Enzymes are chemicals that help the body break down the nutritional parts of the food we eat, including protein, fat and carbohydrates. Once made, enzymes travel through channels (pancreatic ducts) to the small intestine where they break down food.7 In a person with CF, pancreatic ducts can become blocked with mucus, making it harder for enzymes to enter the small intestine where they are needed to do their job.7
Pancreatic ducts can become blocked with mucus
Without these enzymes in the small intestine, the body has trouble breaking down food and absorbing vital nutrients. This can lead to:
- Poor growth, delayed puberty and slow weight gain, even if a lot of food is eaten3,4
- Smelly, large faeces or constipation3,4
Alongside medication such as enzyme tablets, many people with CF are advised to follow a CF-specific diet to help them get the nutrients they need and to manage any digestive symptoms.7

Cystic fibrosis-related diabetes (CFRD)
In the UK, around 35% of adults with CF are reported to receive treatment for CFRD.8 As people with CF get older, damage to their pancreas can mean it stops producing enough insulin, a hormone that helps the body manage glucose levels in the blood. When a person doesn’t have enough insulin, they may develop diabetes.7
Some people with CFRD may find they need to drink and urinate more, feel very tired, lose weight or have trouble gaining weight. They may also experience increased coughing, wheezing or difficulty breathing. However, other people with CFRD may not experience any symptoms.9
Other digestion-related symptoms
People with CF may experience a variety of digestive problems, which may result in:
Weight fluctuation
Some people with CF may experience weight loss, or struggle to gain weight for various reasons. These might include reduced flow of pancreatic enzymes to the small intestine making it hard to release the nutrients from food and, for those with CFRD, not being able to use the sugar from the foods they eat4,7,9
Distal intestinal obstruction syndrome (DIOS)
Some people with CF may produce stools that are thicker than usual because they have difficulties digesting food. This can block the small intestines, causing pain and nausea. DIOS treatment varies depending on the severity of the symptoms and obstruction10
Gastro-oesophageal reflux disease (GORD)
GORD is very common in people with CF and occurs when stomach acid travels upwards into the oesophagus (the tube that connects the mouth to the stomach). This may cause a heartburn sensation, pain and/or swelling7
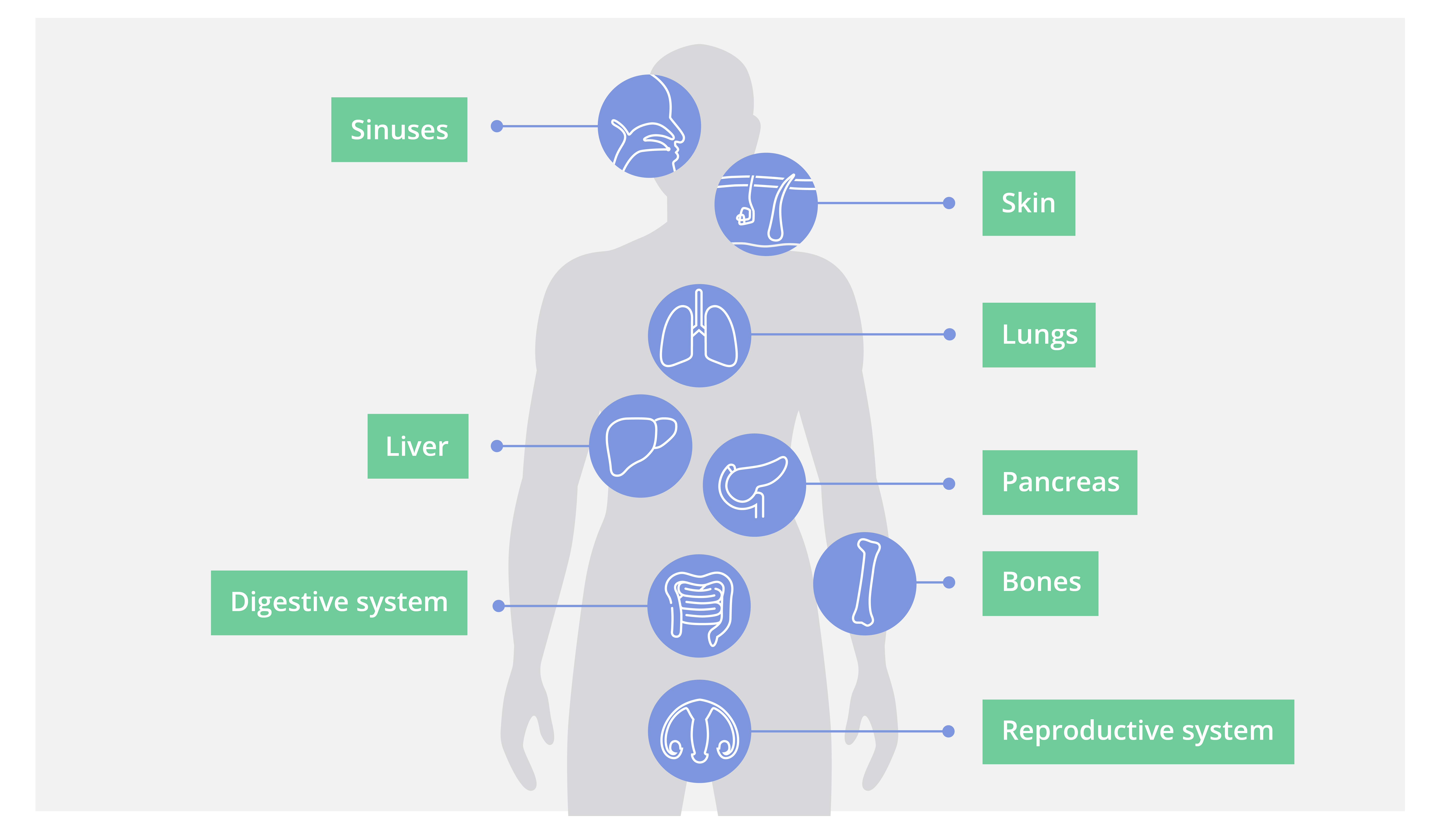
How CF affects other body parts
Sinuses11

People with CF may have more nasal polyps (fleshy growths inside their nose) than is usual. Nasal polyps and mucus build-up may lead to infection and sinusitis (the inflammation or swelling of the sinuses). This may cause a blocked nose, headaches, cough and in some cases the loss of smell
Skin
- Sweat of people with CF contains more salt that normal, which crystallises and can be visible on the skin11
- Normally, the CFTR protein reabsorbs salt before it reaches the skin surface. However, in people with CF, CFTR protein dysfunction may mean salt is not reabsorbed as it should be11
- A few people with CF may also experience skin irritation (rash or dermatitis). This is thought to be influenced by diet and a reduced ability to absorb nutrients from food12
Cirrhosis of the liver13

- The liver plays an important role in processing nutrients and keeping the blood clean and free from harmful substances
- The liver contains many small tubes. In CF, these may become blocked causing irritation and scarring. This scarring is known as cirrhosis, an advanced stage of liver disease
- Cirrhosis makes it harder for the liver to work properly
Reproductive system14
- Although a man with CF can make sperm, the tubes that the sperm travels through may not have formed or be clogged with mucus. This may mean that although intercourse is normal, a man with CF may deliver little or no sperm
- Although a small percentage of men with CF may be able to conceive naturally, 98% are infertile
- In women with CF, thick sticky mucus in the reproductive system may reduce fertility
Reduced bone density15
- As people with CF age, they may be at risk of reduced bone density (weakened bones) and fractures. This is thought to be the result of a number of factors including poor nutritional status (particularly reduced vitamin D levels)
- It is important that those living with CF follow a healthy balanced diet that is tailored to individual needs. Check with your doctor, nurse or dietician for specific CF dietary advice
-
Informed Health. How do lungs work? Available at: https://www.ncbi.nlm.nih.gov/books/NBK401240/. Accessed July 2024.
-
Richardson M. The physiology of mucus and sputum production in the respiratory system. Nursing Times. 2003;99(23):63–64. Available at: https://cdn.ps.emap.com/wp-content/uploads/sites/3/2003/06/030610The-physiology-of-mucus-and-sputum-production-in-the-respiratory-system.pdf. Accessed July 2024.
-
Cystic Fibrosis Foundation. What is cystic fibrosis? Available at: www.cff.org/What-is-CF/About-Cystic-Fibrosis/. Accessed July 2024.
-
Mayo Clinic. Cystic Fibrosis. Available at: https://www.mayoclinic.org/diseases-conditions/cystic-fibrosis/symptoms-causes/syc-20353700. Accessed July 2024.
-
Goss CH, Burns JL. Thorax 2007;62(4):360–367
-
Cystic Fibrosis Trust. What are the causes of cystic fibrosis? Available at: https://www.cysticfibrosis.org.uk/what-is-cystic-fibrosis/what-causes-cystic-fibrosis. Accessed July 2024.
-
Cystic Fibrosis Foundation. The digestive tract. Available at: https://www.cff.org/managing-cf/digestive-tract. Accessed July 2024.
-
Cystic Fibrosis Trust. UK Cystic Fibrosis Registry: 2020 Annual Data Report. Available at: https://www.cysticfibrosis.org.uk/sites/default/files/2022-05/2020AnnualDataReportVersion4.pdf. Accessed July 2024.
-
Cystic Fibrosis Foundation. Cystic fibrosis-related diabetes. Available at: https://www.cff.org/managing-cf/cystic-fibrosis-related-diabetes. Accessed July 2024.
-
Cystic-Fibrosis.com. What is distal intestinal obstructive syndrome (DIOS)? Available at: https://cystic-fibrosis.com/clinical/dios. Accessed July 2024.
-
Cystic Fibrosis Trust. Additional symptoms of cystic fibrosis. Available at: https://www.cysticfibrosis.org.uk/what-is-cystic-fibrosis/how-does-cystic-fibrosis-affect-the-body/symptoms-of-cystic-fibrosis/additional-complications. Accessed July 2024.
-
Wenk KS et al. Arch Dermatol 2010;146(2):171–174.
-
Cystic Fibrosis Trust. Liver disease and cystic fibrosis. Available at: https://www.cysticfibrosis.org.uk/what-is-cystic-fibrosis/how-does-cystic-fibrosis-affect-the-body/symptoms-of-cystic-fibrosis/liver-disease. Accessed July 2024.
-
Cystic Fibrosis Trust. Fertility and cystic fibrosis. Available at: https://www.cysticfibrosis.org.uk/what-is-cystic-fibrosis/how-does-cystic-fibrosis-affect-the-body/symptoms-of-cystic-fibrosis/fertility. Accessed July 2024.
-
Cystic Fibrosis Trust. Bone disease and cystic fibrosis. Available at: https://www.cysticfibrosis.org.uk/what-is-cystic-fibrosis/how-does-cystic-fibrosis-affect-the-body/symptoms-of-cystic-fibrosis/bone-disease. Accessed July 2024.



